Mission
To end human suffering from diseases of the ear and lateral skull base.
Our Latest News
Dr. Goldstein at ACI Alliance CI2026 Chicago Conference
Read Article
Cochlear Implant Satisfaction Presentation at CI2026
Read Article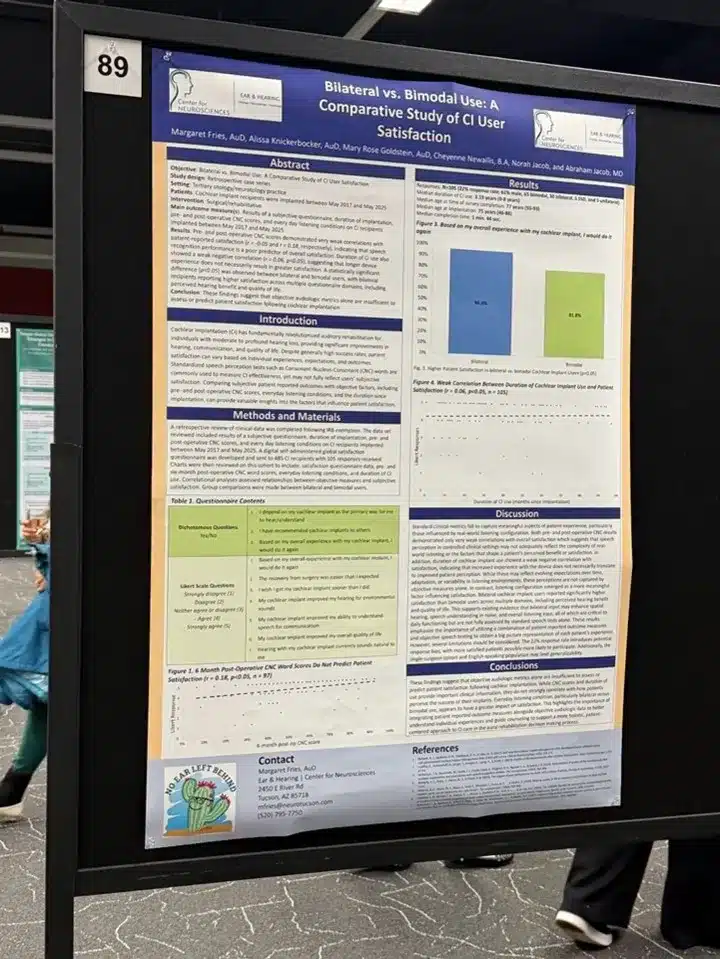
Bilateral CI Users Report Higher Satisfaction than Bimodal Users
Read Article
Click here for the full Ear & Hearing News Article Library
Vision
To provide personalized, compassionate, and state-of-the-art care that generates outstanding clinical outcomes and high patient satisfaction.
With the most experienced otologist/neurotologist in Southern Arizona, three doctors of audiology, personalized clinical coordination, comprehensive hearing and vestibular (balance) testing, a state-of-the-art implantable hearing devices program, and complete infrastructure for clinical research, Ear & Hearing at the Center for Neurosciences provides unmatched care in Southern Arizona for all disorders of the ear and lateral skull base.
Patients are referred to us from across Arizona, New Mexico, southern Texas, portions of Nevada/Colorado, and even parts of California for problems requiring subspecialty otologic, neurotologic, or audiologic expertise. We also welcome self-referrals and second opinions.
To request an appointment, please call (520) 795-7750 or complete the form below.
Otology, Neurotology, and Cranial Base Surgery
As the medical and surgical foundation for Ear & Hearing at the Center for Neurosciences, the Otology, Neurotology and Cranial Base Surgery program offers complete diagnostic care, treatment, and rehabilitation of complex ear diseases. Headed by Dr. Abraham Jacob, fellowship-trained and board-certified in Otology/Neurotology, specific expertise is available for treatment of skull base tumors (vestibular schwannomas/acoustic neuromas as well as posterior cranial fossa meningiomas), facial nerve disorders, primary/revision middle ear and mastoid surgery as well as implantable hearing technologies (cochlear implants, bone anchored hearing aids, and implantable hearing aids).
Otoneurology
Otoneurology is a neurology subspecialty focused on the medical diagnosis and treatment of vertigo, dizziness, imbalance, and eye movement disorders. It is distinct from Neurotology, which is a primarily surgical subspecialty addressing diseases of the ear and lateral skull base. Together, these complementary disciplines allow Ear & Hearing at the Center for Neurosciences to provide comprehensive care across the full spectrum of inner-ear and central vestibular conditions — from peripheral disorders treated medically or surgically to central causes of dizziness requiring neurologic expertise. Dr. Roksolyana Tourkevich leads the Otoneurology program at the Center for Neurosciences. She earned her medical degree and completed her residency training in Neurology at the University of Arizona College of Medicine, followed by a fellowship in Vestibular and Ocular-Motor Oto-Neurology at Johns Hopkins University School of Medicine. Dr. Tourkevich is board-certified by the American Board of Psychiatry and Neurology, speaks fluent Ukrainian, and joined the Center for Neurosciences in 2022. In close partnership with Otology/Neurotology and Audiology, Dr. Tourkevich provides specialized evaluation and management of patients with vertigo, dizziness, imbalance, and eye movement disorders — including conditions in which the cause crosses the boundary between the inner ear and the central nervous system.
Audiology
Audiology, in close partnership with Otology/Neurotology, offers complete hearing health solutions within Ear & Hearing at the Center for Neurosciences. Mary Rose Goldstein, AuD, CCC-A, FAAA, Alissa Knickerbocker, AuD, CCC-A, FAAA and Margaret Fries, AuD, FAAA, providing diagnostic hearing evaluations, tinnitus evaluations, electrophysiologic testing, vestibular evaluations, hearing aid fittings, bone anchored hearing devices, and cochlear implant services for all ages. Our audiologists strive to provide you with accurate information regarding your hearing status, promote understanding of your hearing and communication needs, increase your knowledge of evidence-based management and/or treatment options, and introduce you to the hearing health tools and resources that can maximize your quality of life.
Our Programs
Four integrated programs work together to provide a complete continuum of care, from diagnosis through long-term rehabilitation.
Otology / Diseases of the Ear
Medical and surgical care for the full breadth of ear conditions, including chronic and recurrent ear infections, cholesteatoma, tympanic membrane perforations, otosclerosis (stapes surgery), conductive and sensorineural hearing loss, sudden hearing loss, tinnitus, autoimmune inner ear disease, facial nerve disorders, and ototoxicity monitoring for patients receiving chemotherapy or other ototoxic medications.
Neurotology / Lateral Skull Base Surgery
Specialized management of vestibular schwannoma (acoustic neuroma), posterior fossa and petroclival meningioma, glomus tumors (jugulare and tympanicum), facial nerve tumors, temporal bone encephalocele, petrous apex lesions, and other complex skull base diseases — managed through observation, microsurgery, or stereotactic radiosurgery, individualized to each patient.
Ear-Specific Dizziness
Otoneurologic evaluation and treatment of vertigo and dizziness arising from the inner ear, including benign paroxysmal positional vertigo (BPPV), Ménière’s disease, vestibular neuritis and labyrinthitis, vestibular migraine, and superior semicircular canal dehiscence syndrome.
Audiology
Comprehensive diagnostic audiology and vestibular testing, hearing aid selection and fitting, cochlear implant evaluation and programming, bone-anchored and middle ear implant services, tinnitus evaluation and management, and ototoxicity surveillance — for patients of all ages, including pediatrics and adults with developmental disabilities.
Why Patients Choose Ear & Hearing at CNS
- Complete implantable hearing portfolio. Cochlear implants (Cochlear Americas, MED-EL, Advanced Bionics), bone-anchored hearing devices (Cochlear BAHA, Oticon Ponto), middle ear implants, and Earlens — evaluated, surgically placed, activated, and programmed in-house.
- Comprehensive vestibular and electrophysiologic testing. Videonystagmography (VNG), vestibular evoked myogenic potentials (VEMP), bithermal caloric testing, auditory brainstem response (ABR), electroneurography (ENoG), otoacoustic emissions (OAEs), and ultra-high-frequency audiometry for ototoxicity surveillance.
- Integrated care under one roof. Otology, neurotology, and audiology sit alongside neurology, neurosurgery, neuro-oncology, and radiation oncology within the Center for Neurosciences, enabling seamless multidisciplinary management of conditions such as vestibular schwannoma, facial nerve disorders, and skull base tumors.
- Active clinical research. Our program participates in industry-sponsored and investigator-initiated trials, including in implantable hearing technologies. See our currently enrolling studies.
- Personalized coordination. From your first phone call through long-term follow-up, you work with a consistent, knowledgeable team.
Strategic Partnership with Tucson Ear, Nose & Throat
The Center for Neurosciences and Tucson Ear, Nose & Throat have entered into a strategic partnership to expand the breadth and depth of ear, nose, throat, and skull base care available across Southern Arizona. Patients now benefit from an even broader network of ENT subspecialty expertise.

